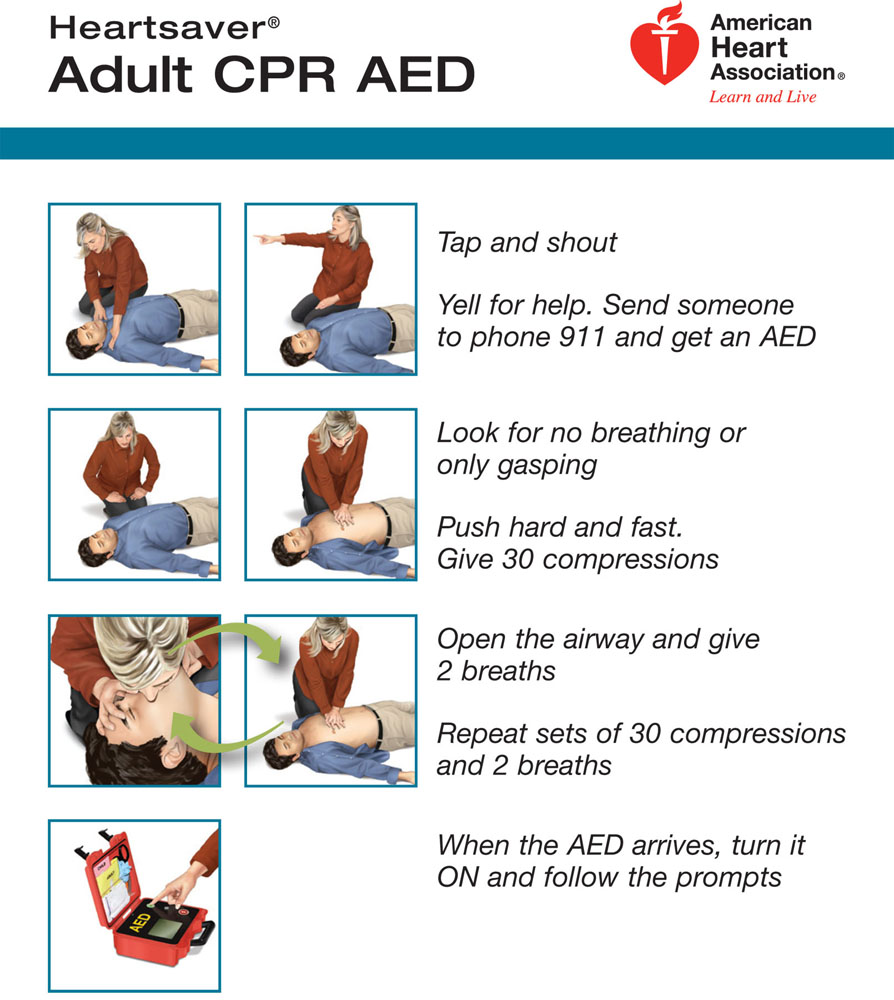
The purpose of this study was to establish how cardiovascular structures known to affect CPR, relate to surface anatomy in patients referred to cardiac magnetic resonance imaging (MRI). The ERC recommendations are regardless of gender, body size, and medical history. As to compression depths, European Resuscitation Council (ERC) decided in 2015 to retain the 2010 guidance that chest compressions should be at least 5 cm but not more than 6 cm, which equates to approximately one-fifth of the adult chest. Compression of the base of the heart or the LVOT might impede forward blood flow, whereas compression of both ventricles avoiding LVOT might be more effective. Previous CT studies have however shown that rather than the left ventricle, structures beneath the INL have been the ascending aorta, the root of aorta, or the left ventricular outflow tract (LVOT). 
According to the cardiac pump theory, direct compression of the ventricles is important. Forward blood flow during CPR is provided by compression of the heart (cardiac pump theory) and/or intra-thoracic pressure fluctuations (thoracic pump theory). Altered hand position might change compression of intrathoracic structures. However, there is little scientific evidence regarding the optimum hand position for chest compressions and the INL is an easily detectible surface landmark. The International Liaison Committee on Resuscitation (ILCOR) recommends placing the hands on the lower half of the sternum and concluded in 2010 that the use of the internipple line (INL) as a landmark for hand placement is not reliable. Conclusionsīased on our study, individualized compression point and depth could be further studied in a prospective, clinical study.Įffectiveness of chest compressions during cardiopulmonary resuscitation (CPR) can be altered by hand position and compression depth, among other components. 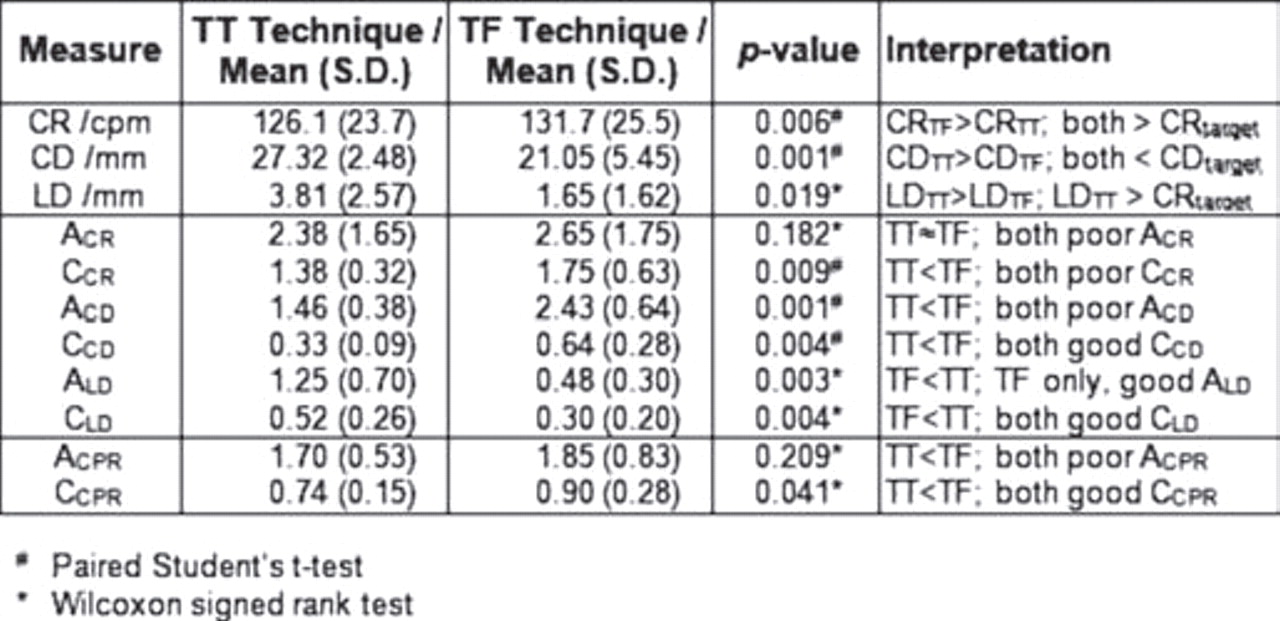
Recommended chest compression depths exceeded the anterior-posterior diameter of blood-filled structures in more than half of the females. LVOT/AV/aortic root was present beneath the origo in almost half the patients with cardiac disease. 
Distance from origo to OCP was 32 (11) mm to the left and 16 (21) mm caudally. AP EXTERNAL for males and females was 25 (2) cm and 22 (2) cm, and AP BLOOD 6.5 cm (2) and 4.7 cm (2), respectively. The structure LVOT/aortic valve (AV)/aortic root was present in 46 % of patients with cardiac disease vs. ResultsĬonsecutive patients, mean (SD), age 52 (17) years, 110 (76 %) males, were categorized: cardiac disease ( n = 74), aortic disease ( n = 13), no findings/study patient (included in another study) ( n = 57). We measured the distance from origo to OCP. We defined OCP based on the image with maximum compressible left and right ventricle and where LVOT was not present. The blood-filled structures beneath origo were identified and the sum of their inner diameters (AP BLOOD) and AP EXTERNAL were measured. We defined origo as the skin surface of the centre of sternum in the internipple line. MRI axial scans of referred patients were analysed. It would work if you were performing hands-only CPR where you were delivering continuous compressions with no interruptions and counting is unnecessary.Using magnetic resonance imaging (MRI) to relate cardiovascular structures to surface anatomy in a population relevant to cardiac arrest victims, relate the external thoracic anterior-posterior (AP) diameter (AP EXTERNAL) and blood-filled structures to recommended chest compression depths, and define an optimal compression point (OCP). You need to be counting to keep track of your compressions. I hear a lot of people suggest you should sing “Stayin Alive” by the Bee Gees to help keep rhythm with your compressions. These 30 compressions should be delivered at a rate of 100-120 compressions per minute. This became a much more efficient way to deliver compressions and breaths for conventional CPR. The 30 compressions created better perfusion of blood carrying oxygen to the heart. Which means you could only deliver 60 compressions in that one minute. With the old standard of 15:2 the most sets you could complete in one minute was 4. Which means if you do the math, you could deliver 90 compressions in that one minute. It also allowed for 3 sets of 30:2 in 1 minute. It also created less interruptions to blood flow, which maintained blood pressure longer. Some of the reasons for changing included making it easier for one person to perform CPR. The American Heart Association adopted the recommended changes also. The old standard of 15 compressions and 2 breaths was changed to 30 compressions to 2 breaths. Because in 2005 when the International Liaison Committee on Resuscitation (ILCOR) updated a lot of the old procedures.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
